
Simeox as a standard of care
At PhysioAssist, we are investing in basic and clinical research to establish Simeox as a standard of care in the airway clearance management of patients suffering from obstructive lung diseases. Clinical validation is essential to achieve this goal and well as to drive coverage in homecare markets.
Published studies
- All
- BE
- CF
- COPD
De Macedo J, Reychler G, Poncin W, Liistro G. Effects of the intermittent intrapulmonary deflation technique on expiratory flow limitation: an in vitro study.
J Clin Monit Comput. 2023 Nov 2. doi: 10.1007/s10877-023-01093-3. Epub ahead of print. PMID: 37917211
READHamidfar R, MurrisEspin M, Mahot M, et al. Feasibility of home initiation of an airway clearance device (SIMEOX) by telecare in people with non-cystic fibrosis bronchiectasis: a pilot study.
BMJ Open Respir Res 2023;10:e001722. doi:10.1136/ bmjresp-2023-001722
READJuliana Ribeiro Fonseca Franco de Macedo, Gregory Reychler, Giuseppe Liistro and William Poncin: Short-Term Effect of Intermittent Intrapulmonary Deflation on Air Trapping in Patients With COPD
Respiratory Care April 2023, 68 (4) 478-487; DOI:
readSands, D.; Walicka-Serzysko, K.; Milczewska, J.; Postek, M.; Jeneralska, N.; Cichocka, A.; Siedlecka, E.; Borawska-Kowalczyk, U.; Morin, L. Efficacy of the Simeox® Airway Clearance Technology in the Homecare Treatment of Children with Clinically Stable Cystic Fibrosis: A Randomized Controlled Trial.
Children 2023, 10, 204.
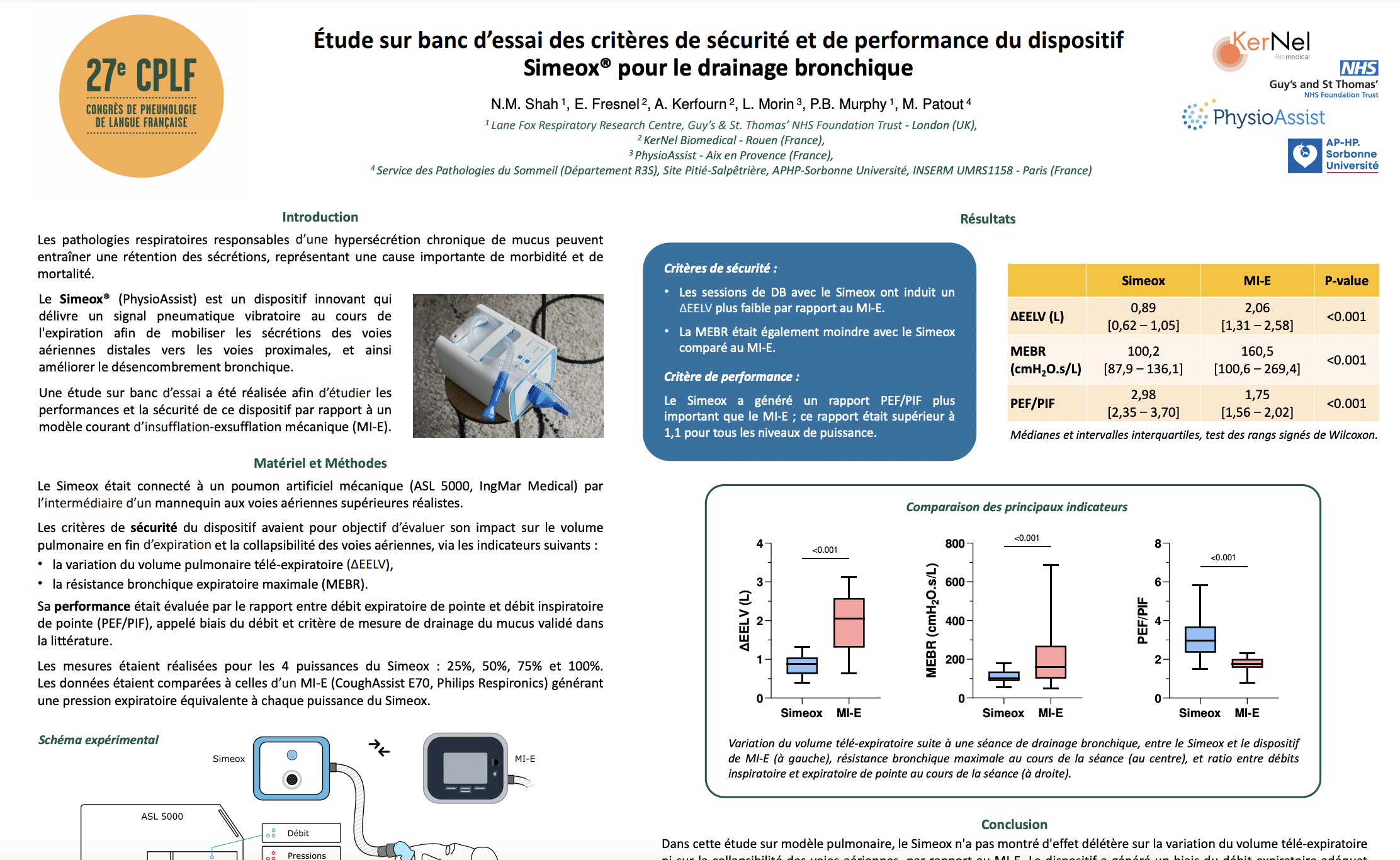
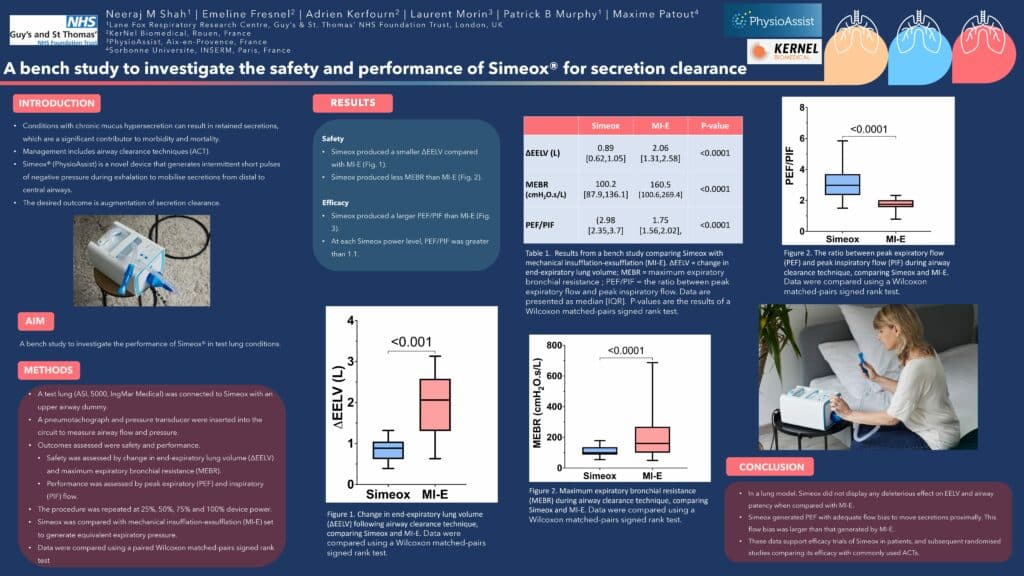
ReadShah NM, Fresnel E, Kerfourn A, Morin L, Murphy PB, Patout M. A bench study to investigate the safety and performance of Simeox for secretion clearance
European Respiratory Journal 2022 60: 3300; DOI: 10.1183/13993003.congress-2022.3300
readSchmidt H, Toth M, Kappler‐Schorn C, Siebeneich U, Bode SFN, Fabricius D. Short‐term effects of a novel bronchial drainage device: a pilot cohort study in subjects with cystic fibrosis.
Health Sci Rep 2022;5:e812. doi.org/10.1002/hsr2.812
ReadHaltenberger, D. und T. Becher: Simeox zu Hause – Patient*innenbefragung zur häuslichen Simeox-Anwendung bei Mukovsizidose/Cystischer Fibrose
Simeox Clincial Notebook 5, 9/2021
ReadK. Walicka-Serzysko, M. Postek, N. Jeneralska, A. Cichocka, J. Milczewska, D. Sands. Addition of a new airway clearance device to chest physiotherapy in children with pulmonary exacerbation of cystic fibrosis.
J Mother Child 2021 Jan 26;24(3):16-24.
ReadLaurent Morin, Damien Marino, Adrien Mithalal. Physiological effects of Simeox Airway Clearance Device in healthy adults
European Respiratory Journal 2020 56: 1274; DOI: 10.1183/13993003.congress-2020.1274
ReadGiovannetti.P, Morin L, Gaubert MR. Safety and Efficacy of an Innovative Airway Clearance Device Versus Manual Chest Physiotherapy Techniques For Airway Secretion Clearance: a Feasibility Study.
European Journal of Respiratory Medicine. 2020; 1(2): 132 - 137 .doi.org/10.31488/ejrm.107
Ivan Solovic, Alena Bodnarova, Laurent Morin. Feasibility and benefits of an innovative airway clearance device in COPD patients hospitalized for acute exacerbation.
European Respiratory Journal 2020 56: 952; DOI: 10.1183/13993003.congress-2020.952
READVitezslav Kolek, Petr Jakubec, Jana Doleželová, Laurent Morin, Jiří Kufa. Feasibility and safety evaluation of Simeox airway clearance technique (ACT) in patients with bronchiectasis.
European Respiratory Journal 2019 54: PA601; DOI: 10.1183/13993003.congress-2019.PA601 (ERS 2019 Poster)
ReadP. Sliwinski, D. Klatka, A. Gladzka, L. Morin, K. Iwan, Benefits of Simeox airway clearance technology in non-CF patients with bronchiectasis
American Journal of Respiratory and Critical Care Medicine 2019; doi.org/10.1164/ajrccm-conference.2019.199.1_MeetingAbstracts.A5720
ReadF. Mihaltan, L. Morin, C. Borcea, A. Costantin, V.-C. Cosei. Evaluation of an Innovative Airway Clearance Technology in Comparison to Manual Chest Physiotherapy in Acute Exacerbation of Chronic Obstructive Pulmonary Disease (COPD).
American Journal of Respiratory and Critical Care Medicine 2019; doi.org/10.1164/ajrccm-conference.2019.199.1_MeetingAbstracts.A3752.
ReadFlorin Mihaltan, Laurent Morin, Corina Borcea, Ancuta Costantin, Alexandru Pahontu, Lucia Marinescu, Valentin-Caius Cosei. Late Breaking Abstract - Effects of a new Airway Clearance Technology versus manual physiotherapy in COPD
European Respiratory Journal 2018 52: PA4047; DOI: 10.1183/13993003.congress-2018.PA4047 (ERS 2018 Poster)
ReadKatarzyna Iwan, Dorota Klatka, Agata Gladzka, Laurent Morin, Pawel Sliwinski. Late Breaking Abstract - Benefits of a low-frequency airway clearance technology in non-CF patients with bronchiectasis.
European Respiratory Journal 2018 52: PA805; DOI: 10.1183/13993003.congress-2018.PA805 (ERS 2018 Poster)
readClinical Documentation



CF DE. SCHMIDT & DR. FABRICIUS (ULM) Health science Report 2022
Read interactive version Download PDF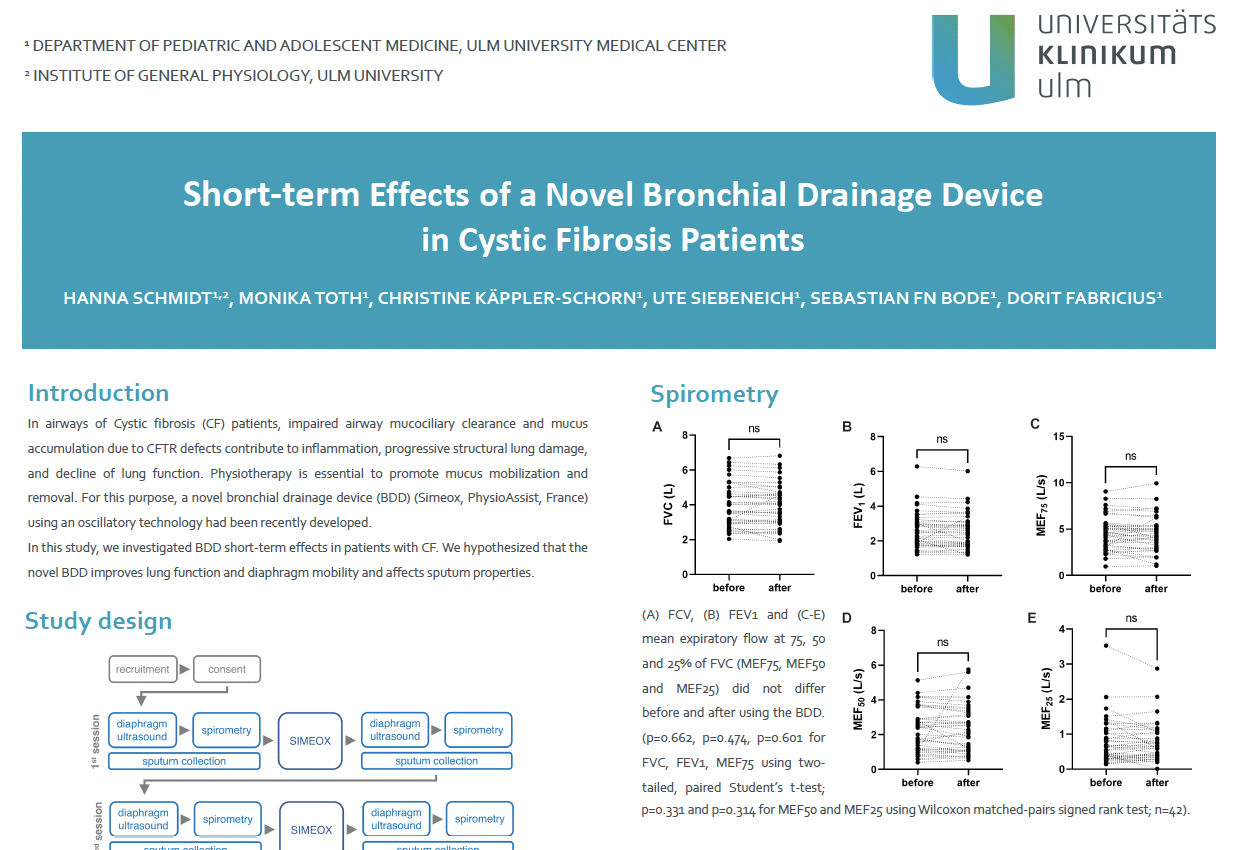
CF / DR SCHMIDT & DR FABRICIUS / ERS 2021
Download PDF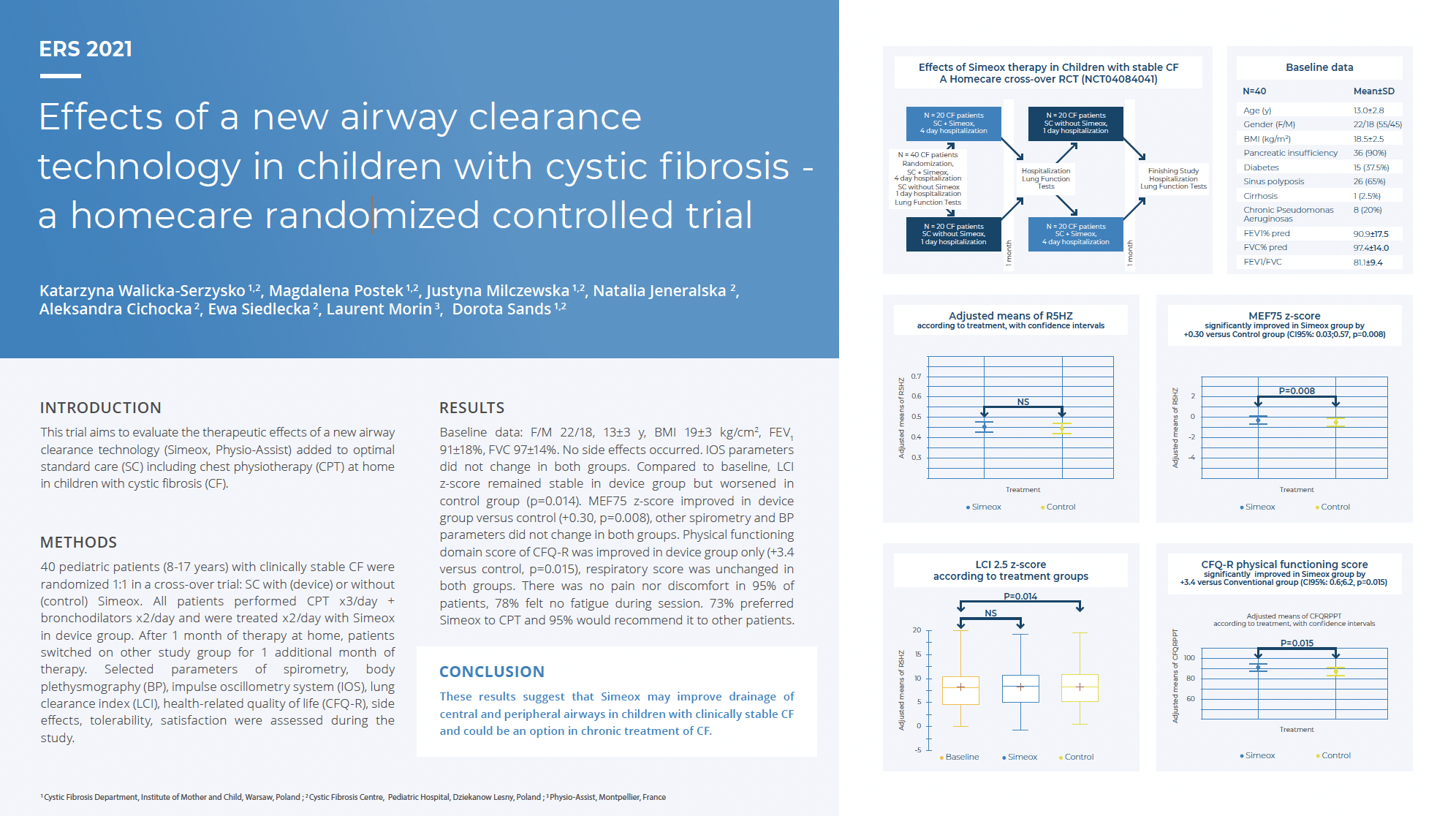
CF / PR SANDS / ERS 2021
Download PDF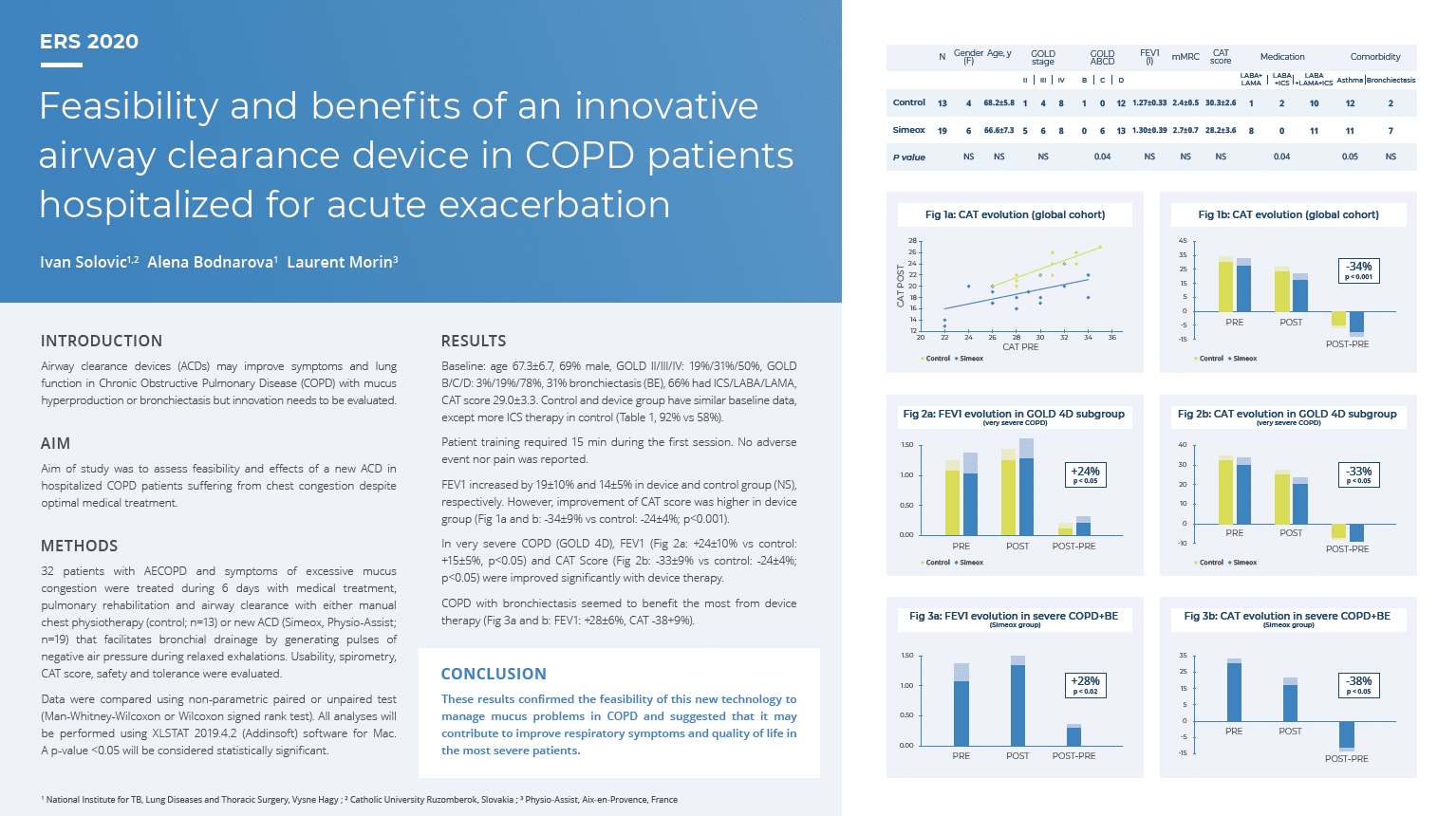
COPD / SOLOVIK ET BODNAROVA / ERS 2020
Download PDF
CF / PROFFIT, MAGNI, DESBOIS, MORIN / ERS 2020
Download PDF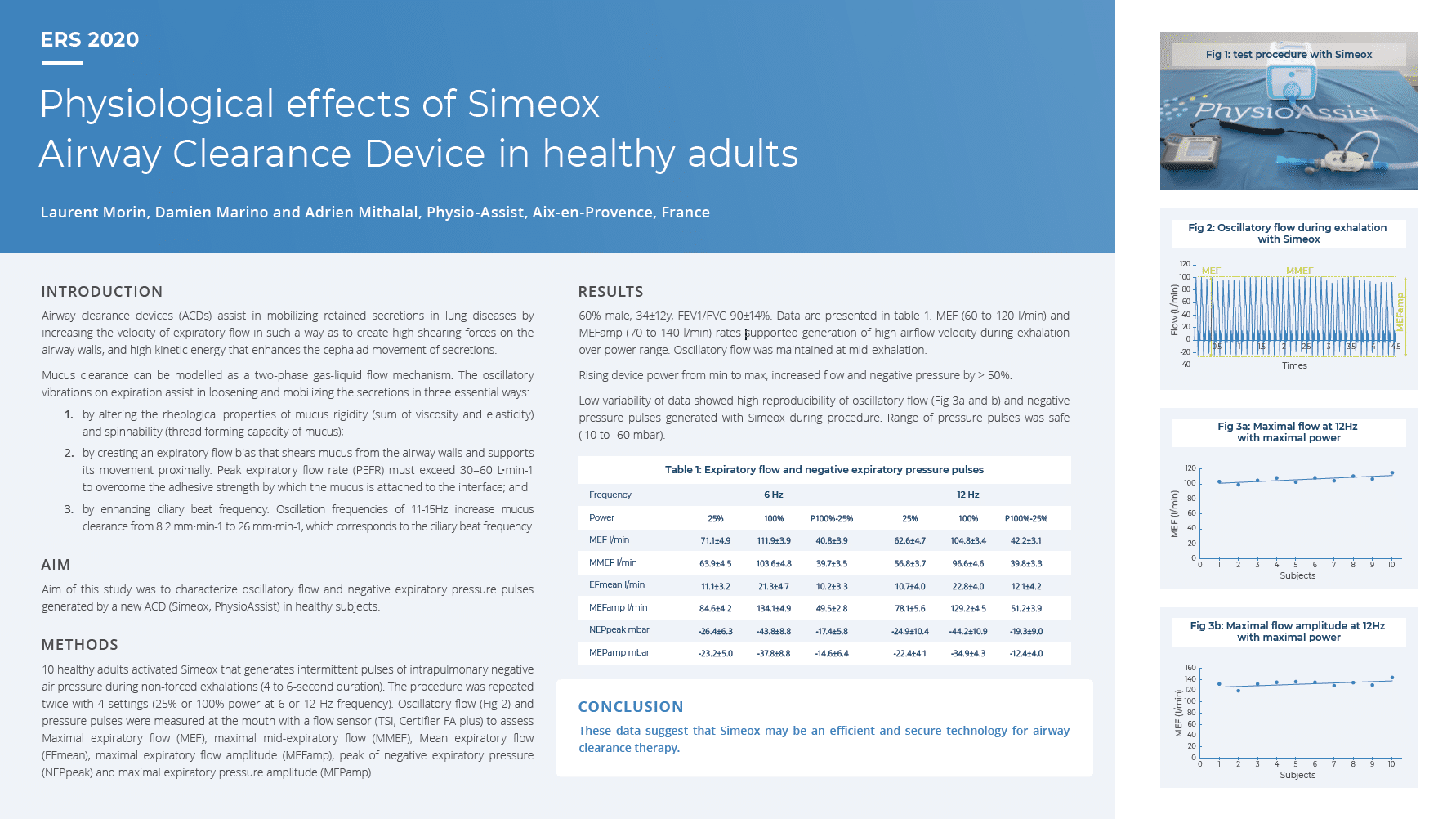
BENCH TEST / ERS 2020
Download PDF
COPD / Mihaltan et al. - ERS 2018 / ATS 2019
Download PDF
COPD / Mihaltan et al. - CPLF 2019
Download PDF
CF / Sands et al. - ECFS 2019
Download PDF
Non CF-BE / Kolek et al, ERS 2019
Download PDF
Non CF-BE / Sliwinski et al. - ERS 2018 / ATS 2019
Download PDF
Clinical Notebook n°2
Download PDF
Clinical Notebook n°3
Download PDF
Clinical Notebook n°4
Download PDF
Clinical Notebook n°5
Download PDFThe expected results
- Mucus that interferes with your breathing is easily mobilised.
- No more waking up at night because of coughing
- You are once again serene when you go out shopping, visit your friends or your family.
- You don’t have to exhaust yourself to get your sputum out.
- You preserve your energy to live the rest of your day to the fullest.
Main Clinical Trials
Mucosim Trial
Impact of Simeox Airway Clearance Device on Respiratory Function and Symptoms in Adult Patients with Cystic Fibrosis.
Multicentric Randomized Controlled Trial.
Primary endpoint: Evolution of Total lung resistance (Airwave Oscillometry System).
Control group: autogenic drainage.
Number of patients : 42 adult patients with CF.
Homecare CF trial
Long Term Efficacy and Acceptability of Simeox Used Autonomously and at Home in Patients With Cystic Fibrosis.
Multicentric Randomized Controlled Trial.
Primary endpoints: Respiratory score domain CFQ-R and FEV1.
Control group: standard care with CPT.
Number of patients: 224 patients with CF > 14 years.
HOMECARE PEDIATRIC CF TRIAL
Efficacy of Simeox Airway Clearance Therapy in Children With Cystic Fibrosis.
Monocentric Randomized Controlled Trial.
Primary endpoint: Evolution of lung resistance (IOS).
Control group: standard care with CPT.
Number of patients: 40 pediatric patients with CF.
Proof of concept trial in CF
Effects of Simeox on Airway Clearance in Cystic Fibrosis.
Monocentric Cross-over Randomized Controlled Trial.
Primary endpoint: Weight of sputum secretion.
Control group: autogenic drainage.
Number of patients: 20 adult patients with CF.
Proof of concept trial in COPD
Effects of Simeox on Static Hyperinflation in Patients With COPD
Monocentric Cross-over Randomized Controlled Trial.
Primary Endpoint: Change in FRC after and 30 min.
Control group: PEP therapy.
Number of partients: 25 adult patients with COPD.
Symposiums / Communications
ERS2022 - Workshop
"A new era in distal mucus management"
EU Virtual Roundtable 1 (Simeox therapy in CF)
Reinforcement of IV therapy - May 2021
EU Virtual Roundtable 2 (Simeox therapy in CF)
Mobilization of mucus during regular care - May 2021
EU Virtual Roundtable 3 (Simeox therapy in CF)
Personalized medicine / Home rehabilitation - May 2021
ERS 2018 Industry Practical Workshop
Key Moments
ERS 2018 Industry Practical Workshop
Full Version
Scientific Session
Pulmonology Congress, Warsaw 2018 - Simeox Technology
Scientific Session
Pulmonology Congress, Warsaw 2018 - Simeox Discussion
Scientific Session
Pulmonology Congress, Warsaw 2018 - Dr Pérez and Mr Gauchez
Scientific Session
Pulmonology Congress, Warsaw 2018 - Prof. Solovic and Mrs Bodnarova
Scientific Session
Pulmonology Congress, Warsaw 2018 - Prof. Mihaltan and Dr Cosei
Scientific Session
Pulmonology Congress, Warsaw 2018 - Dr Elena Amelina
Scientific Session
Pulmonology Congress, Warsaw 2018 - Prof. Paweł Śliwiński
Scientific Session
Pulmonology Congress, Warsaw 2018 - Prof. Vítězslav Kolek
Committee Advisors
Martine Reynaud‑Gaubert
Professor of Medicine and Head of Department Pneumology, rare respiratory disease, cystic fibrosis
Martine Reynaud-Gaubert
Professor of Medicine and Head of Department Pneumology, rare respiratory disease, cystic fibrosis
Hospital Practitioner Hospital north of Marseille - APHM
Medical Officer of Lung Transplant Program Adults
Marseille Coordinator of the Competence Center for Pulmonary Hypertension weans
Coordinator of Resource Center and Competence Cystic Fibrosis (CRCM) Coordinator of Disease Competence Center Rare Lung adult
Professor Reynaud-Gaubert directs clinical studies and PhysioAssist publications since 2011 to produce and develop scientific knowledge of PhysioAssist the benefit of patients.
Hughes Gauchez
Osteopathy physiotherapist specializing in respiratory - CKRF Lille
Hughes Gauchez
Osteopathy physiotherapist specializing in respiratory - CKRF Lille
Referent Physiotherapist for the association “Vaincre la mucoviscidose”
Founding president of the AMK Representative IPGCF for France (International Physiotherapy Group for Cystic Fibrosis)
President of P2R Training - Autogenous drainage and respiratory physiotherapy techniques
Hugues Gauchez accompanies Physio-Assist in defining the Simeox use patterns by physiotherapists. He is an expert autogenous drainage and adopts Simeox into daily practice, in assisted sessions or during patient autonomy implementation.
Sophie Jacques
Respiratory Physiotherapist - Rennes
Sophie Jacques
Respiratory Physiotherapist - Rennes
Autogenous drainage trainer in France, Belgium and Eastern countries
President of the French Association “Mucoviscidose et Kinésithérapie” (AMK)
Respiratory Rehabilitation Inter-Universities Diploma
Sophie Jacques uses Simeox with her patients in her daily practice and helps them to autonomously manage their drainage. Sophie helps Physioassist with the Simeox training, she brings and shares her Simeox expertise with new physiotherapist users.
Mathilde Proffit
Respiratory Physiotherapist, La Bulle, NICE
Mathilde Proffit
Junior trainer in autogenic drainage in France and Eastern Europe, lecturer in respiratory specialties at the Physiotherapy Schools of Nice and Saint Michel - Paris.
University graduations speciality paediatrics Paris Descartes / Stetho-acoustic training / pulmonary ultrasound / paediatric manual therapy / medical hypnosis / yoga teacher
Mathilde worked at the Cystic Fibrosis Center of the Necker Enfants Malades University Hospital, Paris - where she started using Simeox on various patients, both paediatric and adult, some with very severe pulmonary conditions. She now practices in Nice in her respiratory rehabilitation practice - La Bulle, and uses Simeox with all her patients.
She has a great deal of experience with Simeox, having used it for over 3 years, with consistently excellent clinical results.
Testimonials
COPD
Colette, France
Bronchiectasis
Fabienne, France
COPD
Nadine, France
Cystic fibrosis
Sarah, Germany
Cystic fibrosis
Perrine, France
COPD
Marie-Claude, France
COPD
Yves, France
Cystic fibrosis
Antoine, France
Dyspnea - COPD
Cystic fibrosis
Alice, France
Bronchial drainage - COPD
Simeox Testimony
Lysianne, France
Simeox Testimony
Gil, France
Simeox Testimony
Michèle, France
Simeox Testimony
Ghislaine, France